1948 – 2020
72 years young
Click a year to discover what we’ve achieved since 1948
1940s 1950s 1960s 1970s 1980s 1990s 2000s 2010s
1940s
1948
NHS established

The NHS is born on July 5 1948 out of a long-held ideal that good healthcare should be available to all, regardless of wealth. When health secretary Aneurin Bevan opens Park Hospital in Manchester it is the climax of a hugely ambitious plan to bring good healthcare to all. For the first time hospitals, doctors, nurses, pharmacists, opticians and dentists are brought together under one umbrella organisation that is free for all at the point of delivery. The central principles are clear: the health service will be available to all and financed entirely from taxation, which means that people pay into it according to their means.
1950s
1952
Prescription charges introduced

Prescription charges of one shilling (5p) are introduced and a flat rate of a pound for ordinary dental treatment is also brought in on June 1 1952. Prescription charges are abolished in 1965, and prescriptions remain free until June 1968 when the charges are reintroduced.
1953
DNA structure revealed

On April 25 James D Watson and Francis Crick, two Cambridge University scientists, describe the structure of a chemical called deoxyribonucleic acid in Nature magazine. DNA is the material that makes up genes which pass hereditary characteristics from parent to child. Crick and Watson begin their article: “We wish to suggest a structure for the salt of deoxyribonucleic acid (DNA). This structure has novel features which are of considerable biological interest.” DNA allowed the study of disease caused by defective genes.
1954
Smoking – cancer link established

Sir Richard Doll establishes a clear link between smoking and lung cancer. In the 1940s, British scientist Doll begins research into lung cancer after incidences of the disease rise alarmingly. He studies lung cancer patients in 20 London hospitals, and he expects to reveal that the cause is fumes from coal fires, car fumes or Tarmac. His findings surprise him and he publishes a study in the British Medical Journal, co-written with Sir Austin Bradford Hill, warning that smokers are far more likely than non-smokers to die of lung cancer. Doll gives up smoking two-thirds of the way through his study and lives to be 92.
1954
Children get daily visits

Daily visits gradually introduced for children who until now had been allowed to see parents only at the weekend. Until now children in hospital are often only allowed to see their parents for an hour on Saturdays and Sundays and are frequently placed in adult wards, with little attempt to explain to them why they are there or what is going to happen. Paediatricians Sir James Spence in Newcastle and Alan Moncriff at Great Ormond Street are making considerable steps to change this, demonstrating that such separation is traumatic for children. As a result, daily visiting is introduced gradually.
1956
The Graduate Scheme

The NHS Graduate Management Trainee Scheme was first launched in 1956. Graduates were offered a two-year intensive training programme. The scheme would produce many of the NHS’s senior leaders over the next few decades, including Sir David Nicholson and Simon Stevens.
1958
Polio and diphtheria vaccinations
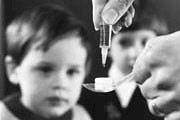
A programme to vaccinate everyone under the age of 15 against polio and diphtheria is launched. One of the primary aims of the NHS is to promote good health, not simply to treat illness, and the introduction of the polio and diphtheria vaccine is a key part of the NHS’s plans. Before this programme, cases of polio could climb as high as 8,000 in epidemic years, with cases of diphtheria as high as 70,000, leading to 5,000 deaths. This programme sees everyone under the age of 15 vaccinated and will lead to an immediate and dramatic reduction in cases of both diseases.
1960s
1960
First kidney transplant
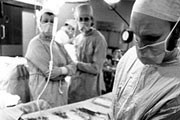
An Edinburgh doctor, Michael Woodruff, performs the first UK transplant involving an identical set of twins. The first UK transplant takes place at Edinburgh Royal Infirmary on October 30 and involves a set of 49-year-old twins. The procedure is a success, with both donor and recipient living for a further six years before dying of an unrelated illness. Kidney transplants, which for many are a welcome alternative to a lifetime of regular dialysis, now enjoy a high success rate but demand outstrips supply due to an ageing population meaning an increased incidence of renal failure, while the number of donor organs available has fallen.
1960
First hip replacement
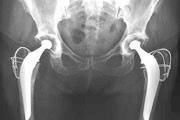
First full hip replacement is carried out by Professor John Charnley in Wrightington Hospital. Charnley begins to devote his energies to developing full hip replacements from 1958 and moves to the Wrightington Hospital where the first full hip replacement takes place. He asks his patients if they mind giving back the hip post-mortem. Apparently 99% of them agree, so his team would regularly collect the replacement hips to check wear and tear, and aid research. He improves his design with a low-friction hip replacement, and in November 1962 the modified Charnley hip replacement becomes a practical reality.
1961
Contraceptive pill
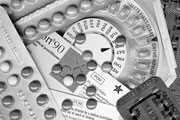
The contraceptive pill is made widely available and is hailed as a breakthrough of the 20th Century. The launch of the contraceptive pill, which suppresses fertility with either progesterone or oestrogen or, more commonly, a combination of both, plays a major role in women’s liberation and contributes to the sexual freedom of the so-called Swinging Sixties. Initially, it is only available to married women, but this is relaxed in 1967. Between 1962 and 1969, the number of women taking the Pill will rise dramatically, from approximately 50,000 to 1m.
1962
The Hospital Plan

Porritt Report is published and results in Enoch Powell’s Hospital Plan. The medical profession criticises the separation of the NHS into three parts – hospitals, general practice and local health authorities – and calls for unification. The Hospital Plan approves the development of district general hospitals for population areas of about 125,000. The 10-year programme is new territory for the NHS and it soon becomes clear that it has underestimated the cost and time taken to build new hospitals. But with the advent of post-graduate centres, nurses and doctors will be given a better future.
1967
The Salmon Report

This major report makes recommendations for the development of senior nursing staff. The Salmon Report is published and sets out recommendations for developing the nursing staff structure and the status of the profession in hospital management. The Cogwheel Report considers the organisation of doctors in hospitals and proposes speciality groupings. It also highlights the efforts being made to reduce the disadvantages of the three-part NHS structure – hospitals, general practice and local health authorities – acknowledging the complexity of the NHS and the importance of change to meet future needs
1967
Abortion Act
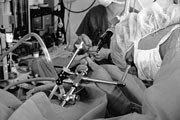
The Abortion Act is introduced by Liberal MP David Steel and is passed on a free vote, becoming law on April 27 1968. This new act makes abortion legal up to 28 weeks if carried out by a registered physician and if two other doctors agree that the termination is in the best mental and physical interests of the woman. In 1990, the time limit is lowered to 24 weeks. The act does not extend to Northern Ireland.
1968
Sextuplets born
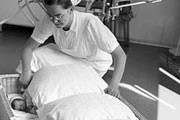
Sextuplets born after British woman receives fertility treatment. In the morning of October 2 Sheila Thorns celebrates her birthday by undergoing a caesarean section at Birmingham Maternity Hospital. She gives birth to six children, four boys and two girls, but sadly one of the girls dies shortly afterwards. With 28 medical staff at the delivery, the five surviving babies – Ian, Lynne, Julie, Susan and Roger – are cared for by a specialist team. Doctors say around one birth in 3,000m will result in sextuplets. Mrs Thorns had been treated with the fertility treatment gonadotrophin which contains two hormones known as FSH and LH.
1970s
1970
CT scans introduced
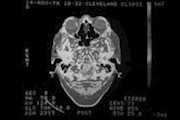
Computer tomography scans start to revolutionise the way doctors examine the body. These scanners produce 3-D images from a large series of two-dimensional X-rays and the first one is started in 1967 by Godfrey Newbold Hounsfield, with his research reaching fruition now. His concept will go on to win him a Nobel Prize, which he will share with the American Allan McLeod Cormack, who developed the same idea across the Atlantic. Since that initial invention, CT scanners have developed enormously, but the principle remains the same.
1972
Endorphins discovered
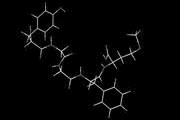
The morphine-like chemicals in the brain called endorphins are discovered. John Hughes and Hans Kosterlitz of Scotland isolate from the brain of a pig what they called enkephalins and will later be termed ‘endorphin’ from an abbreviation of ‘endogenous morphine’. These are polypeptides produced by the pituitary gland and the hypothalamus in vertebrates, and they resemble opiates in their abilities to produce analgesia and a sense of well-being. In other words, they might work as natural pain killers.
1978
First test-tube baby

Louise Brown is the world’s first baby to be born as a result of in-vitro fertilization. The world’s first test tube baby is born on July 25. Parents Lesley and John Brown had failed to conceive due to Lesley’s blocked fallopian tubes. This new technique developed by Dr Patrick Steptoe, a gynaecologist at Oldham General Hospital, and Dr Robert Edwards, a physiologist at Cambridge University found a way to fertilize the egg outside the woman’s body before replacing it in the womb.
1980s
1980
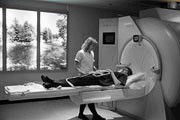
MRI scans introduced
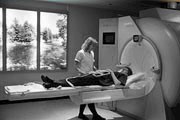
Using a combination of magnetism and radio frequency waves, MRI scanners provide information about the body. Magnetic resonance imaging scanners prove more effective in providing information about soft tissues, such as scans of the brain. The patient lies inside a large cylindrical magnet and extremely strong radio waves are then sent through the body. It provides very detailed pictures, so is particularly useful for finding tumours in the brain; it can also identify conditions such as multiple sclerosis and the extent of damage following a stroke.
1981
Improved health of babies
The 1981 Census shows that 11 babies in every 1,000 die before the age of one. In 1900 this figure was 160. Childhood survival has been revolutionised by vaccination programmes, better sanitation and improved standards of living, resulting in better health of both mother and child. Increased numbers of births in hospital has meant that where unexpected problems do occur, medical help is on hand. Around one baby in eight requires some kind of special care following birth. Twenty years ago, only 20% of babies weighing less than 1,000g (2lbs 2oz) at birth survived. Now that figure is closer to 80%.
1986
AIDS health campaign

The government launches biggest public health campaign in history to educate people about the threat of Aids as a result of HIV. Following a number of high-profile deaths, the advertising campaign sets out to shock – with images of tombstones and icebergs, followed early in 1987 by a household leaflet, “Don’t die of ignorance”. This was very much in keeping with the NHS’s original concept that it should improve health and prevent disease, rather than just offer treatment.
1987
Heart, lung and liver transplant

First heart, lung, and liver transplant are carried out at Papworth Hospital. Professor Sir Roy Calne and Professor John Wallwork carry out the world’s first liver, heart and lung transplant at Papworth Hospital in Cambridge. Professor Calne describes the patient as “plucky” and she survives for a further 10 years after the procedure.
1988
Breast screening is introduced

Comprehensive national breast-screening programme introduced. To reduce breast cancer deaths in women over 50 this project is launched with breast-screening units around the country providing mammograms. A mammogram works by taking an X-ray of each breast, which can show changes in tissue that might be otherwise undetectable. This means that any abnormalities show up as early as possible, making treatment more effective. Screening, together with improved drug therapies will help to cut breast cancer deaths by more than 20%, a trend that looks set to continue.
1990s
1990
NHS and Community Care Act

Internal market is introduced, which means health authorities manage their own budgets. Now health authorities will manage their own budgets and buy healthcare from hospitals and other health organisations. In order to be deemed a “provider” of such healthcare, organisations will become NHS Trusts, that is, independent organisations with their own managements.
1991
Fifty-seven NHS trusts are established to make the service more responsive to the user at a local level. New NHS Trusts will aim to encourage creativity and innovation and challenge the domination of the hospitals within a health service that is increasingly focused on services in the community.
On 16 October 1991, the Secretary of State for Health announced an additional 99 trusts would be established from 1 April 1992 and an additional four London teaching hospitals would be established from 1 April 1993.
1994
NHS Organ Donor Register

National register for organ donation is set up to co-ordinate supply and demand after a five-year campaign. The NHS Organ Donor Register is launched following a five-year campaign by John and Rosemary Cox. In 1989 their son Peter died of a brain tumour. He had asked for his organs to be used to help others. The Coxes said that there should be a register for people who wish to donate their organs. By 2005 more than 12m had registered. Organ donation is needed as demand outstrips supply and this register ensures that when a person dies they can be identified as someone who has chosen to donate their organs.
2000s
2000
NHS walk-in centres
New health facilities open offering convenient access, round-the-clock, 365 days a year. NHS walk-in centres (WiCs) offer convenient access to a range of NHS services and are managed by Primary Care Trusts. There are around 90 NHS WiCs dealing with minor illnesses and injuries. WiCs are predominantly nurse-led first-contact services available to everyone without making an appointment or requiring patients to register. Most centres are open 365 days a year and are situated in convenient locations that give patients access to services even beyond regular office hours.
2002
Primary care trusts launched

Primary care trusts are set up to improve the administration and delivery of healthcare at a local level. The primary care trusts oversee 29,000 GPs and 21,000 NHS dentists. Primary care trusts that are in charge of vaccination administration and control of epidemics also control 80 per cent of the total NHS budget. They also liaise with the private sector when contracting out of services is required. As local organisations, they are best positioned to understand the needs of their community, so they can make sure that the organisations providing health and social care services are working effectively.
2007
Robotic intervention
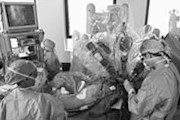
Introduction of robotic arm leads to groundbreaking operations to treat patients for fast or irregular heartbeats. This technological revolution is being used at St Mary’s Hospital, London, and is less risky than more invasive techniques. It works by inserting several fine wires into a vein in the groin, which are then guided to the heart where they deliver an electric current to parts of the heart muscle. Cardiologists control the robot arm via a computer and joystick, but in the future the system could be automated. Around 50,000 people develop an irregular heartbeat each year, and it is a major cause of strokes and heart attacks.
2008
60 years of the NHS

Huge strides have been made by both the health service and the nursing profession in the last 60 years. Nurses are no longer seen as the doctors’ handmaiden. Instead they are leaders and innovators in the service. They are diagnosing, prescribing and designing new services to provide more holistic care. All these achievements have meant a better service for patients – a feat that is undoubtedly worth celebrating.
2009
NHS constitution was published
The NHS belongs to the people. It is there to improve our health and well-being, supporting us to keep mentally and physically well, to get better when we are ill and, when we cannot fully recover, to stay as well as we can to the end of our lives. It works at the limits of science – bringing the highest levels of human knowledge and skill to save lives and improve health. It touches our lives at times of basic human need, when care and compassion are what matter most.
2010s
2010
White Paper: “Equity and Excellence: Liberating the NHS”

On 12 July 2010 a White Paper – ‘Equity and Excellence: Liberating the NHS’ – was published. This has been described as the biggest change to the NHS since its creation in 1948 and contains far reaching and ambitious proposals to change the way in which the service is structured and services are commissioned. In his speech to the House of Commons, Andrew Lansley said that the aim of the White Paper is to put patients at the heart of the service, to put clinicians in the driving seat on decisions about services and to focus the NHS on delivering health outcomes comparable with, or better than, those of our international neighbours.
2011
Health and Social Care Bill

The Bill went for its first reading in the House of Commons on 19th January 2011. The Bill proposes to create an independent NHS Board, promote patient choice, and to reduce NHS administration costs. The Bill is intended to put into effect the policies requiring primary legislation that were set out in the White Paper Equity and Excellence: Liberating the NHS, which was published in July 2010.
2012
On 27 December 2012, a surgical team at Leeds General Infirmary carried out the UK’s first hand transplant operation. The operation involved amputating Mark Cahill’s hand and then transplanting a donor hand during the same operation.
As well as being a first for the UK, it was also the first time a recipient’s hand has been amputated during an operation to attach a donor hand.
The fresh cut, made where you would wear a watch, allowed surgeons to connect nerves in Mr Cahill’s arm with those in the donor hand with great precision – along with the bone, blood vessels and tendons.
2013
The new NHS

The NHS is undergoing major changes in its core structure to deliver the ambitions set out in the Health and Social Care Act. Public Health England, the NHS Trust Development Authority and Health Education England took on their full range of responsibilities at the same time. NHS England is an independent body, separated from the government. Its main aim is to improve health outcomes for people in England. It will do this by creating the culture and conditions for health and care services and staff to deliver the highest standard of care and ensure valuable public resources are used effectively to get the best outcomes for society now and for future generations.
2016
2016 marks the 60th anniversary of the NHS Graduate Management Training Scheme where just 12 people were on the first ever intake. Over the years, the Scheme has produced several leaders and has made a huge impact on the nation’s health service, including Sir David Nicholson and Simon Stevens. The scheme continues to thrive and produce quality leaders for the future of the NHS
2018
70 years of the NHS

The National Health Service turned 70 on 5 July 2018. This provided the perfect opportunity to celebrate the achievements of one of the nation’s most loved institutions, to appreciate the vital role the service plays in everyone’s lives, and to recognise and thank the extraordinary NHS staff – the everyday heroes – who are there to guide, support and care for people, day in, day out.